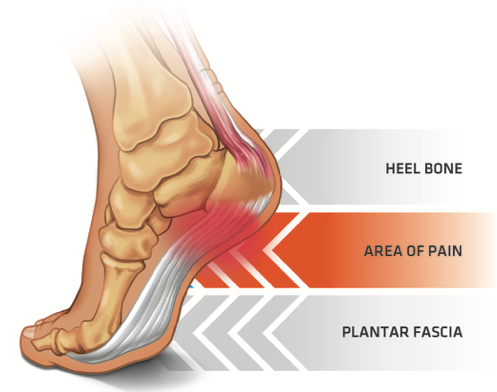
Plantar Fasciitis (Heel Pain)
/What is Plantar Fasciitis?
Inflammation or tearing of the tense band of fibres situated on the sole of the foot.
What does the Plantar Fascia do?
It assists in holding up the arch of the foot in conjunction with other supporting ligaments. It also assists in protecting the foot from piercing injuries when walking barefoot as it is made up of a combination of strong collagen bands interspersed with a layer of fat padding.
What causes Plantar Fasciitis?
· Sports that place additional stress on the heel bone due to running on the toe rather than the heels
· Working in a job that requires excessive walking or standing on a hard surface
· Structure of the foot eg. flat feet, high arches, tight calf muscles or achilles
· Incorrect footwear that doesn’t provide adequate support or cushioning
· Carrying excess weight places extra strain on the Plantar Fascia
· Ageing
How do I know if I have Plantar Fasciitis?
Symptoms may emerge gradually with the prime characteristic being stiffness and difficulty walking after prolonged sitting or immobility. Generally, this eases after a few minutes. There is often a focal, localised pain concentrated on the heel at the rear end of the foot arch.
What investigations do I need to confirm this is my problem?
A clinical examination performed by your physiotherapist to check for tenderness in your foot and the exact location of the pain to make sure that it’s not caused by a different foot problem.
An ultrasound scan or MRI can be used to confirm the diagnosis and will also identify whether there is a partial tear of the fibres of the planter fascia where repeated stress may have caused breakdown of the tensile tissue. These investigations or an x-ray will also identify whether a calcaneal (heel) spur exists. A heel spur results from repeated traction trauma to the heel attachment site of the plantar fascia resulting in gradual deformation of the bone.
How is Plantar Fasciitis treated?
Firstly, the acute inflammatory response that is causing pain and dysfunction needs to be addressed. Standard anti-inflammatory methods are generally useful including the use of ice, rest from provocative activities, the use of protective footwear. Specific stretches are frequently utilised and anti-inflammatory medication may be indicated if approved by your medical practitioner.
The underlying biomechanics that may be causing the problem also need to be assessed. Important considerations include tight calves and excessive pronation (flattening) of the arch of the foot.
*Early physiotherapy intervention is indicated so that you can continue to enjoy life and activity without pain.